Navigating the Complex Landscape of Hospital Compliance: A Guide to EOC, Life Safety, & NFPA Regulations for Patient Care
DECEMBER 2023
By Jody Randall MSN, RN, CIC, HACP-CMS, HACP-PE
CEO and Founder
In the ever-evolving landscape of healthcare, ensuring hospital compliance is not just a regulatory requirement but a commitment to providing a safe and secure environment for patients, staff, and visitors. This blog aims to delve into the intricacies of hospital compliance, focusing on the crucial aspects of Environment of Care (EOC), Life Safety, and the National Fire Protection Association (NFPA) regulations that collectively shape the framework for patient care facilities.
1. Understanding Environment of Care (EOC):
- Definition and Scope: What constitutes the Environment of Care in a hospital setting? Discuss the various elements such as safety, security, hazardous materials, and emergency management.
- Joint Commission Standards: Explore the role of The Joint Commission in setting EOC standards and the impact on hospital accreditation.
- Compliance Challenges: Highlight common challenges faced by hospitals in maintaining EOC compliance and strategies to overcome them.
2. Life Safety in Healthcare Facilities:
- Regulatory Overview: Provide an overview of the Life Safety Code (NFPA 101) and its significance in healthcare settings.
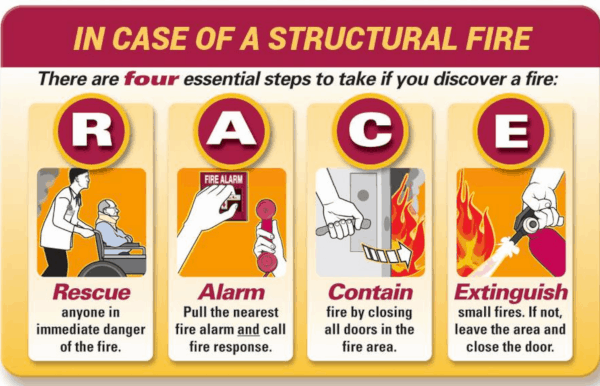
- Fire Prevention and Preparedness: Discuss the specific measures hospitals must take to prevent and respond to fire emergencies, including fire drills, evacuation plans, and fire safety training.
- Building Design and Construction: Explore how hospital infrastructure must adhere to Life Safety Code requirements, covering areas such as egress routes, fire barriers, and smoke control.
3. NFPA Regulations and Healthcare:
- NFPA 99 (Health Care Facilities Code): Delve into NFPA 99, focusing on its application to healthcare facilities, including electrical systems, gas and vacuum systems, and medical gas requirements.
- Integration with EOC: Discuss how NFPA regulations align with and complement the broader Environment of Care framework to enhance overall safety and compliance.
- Recent Updates and Emerging Trends: Provide insights into any recent updates to NFPA codes relevant to healthcare facilities and discuss emerging trends in compliance and safety standards.
4. Patient Care Implications:
- The Intersection of Compliance and Patient Care: Analyze how adherence to EOC, Life Safety, and NFPA regulations directly impacts the quality of patient care.
- Case Studies: Share real-world examples where compliance failures have affected patient outcomes and emphasize the importance of a holistic approach to healthcare management.
5. Best Practices and Recommendations:
- Developing a Robust Compliance Program: Offer practical advice on establishing and maintaining a comprehensive hospital compliance program.
- Training and Education: Emphasize the role of ongoing training and education for staff to ensure awareness and understanding of compliance requirements.
- Continuous Improvement: Discuss the concept of continuous improvement in the context of compliance, encouraging hospitals to adapt to evolving regulations and industry best practices.
In the complex and highly regulated world of healthcare, navigating the intricacies of Environment of Care, Life Safety, and NFPA regulations is essential for ensuring the well-being of all stakeholders. By understanding the interplay between these elements, hospitals can not only meet regulatory requirements but also foster a culture of safety, ultimately enhancing the quality of patient care.